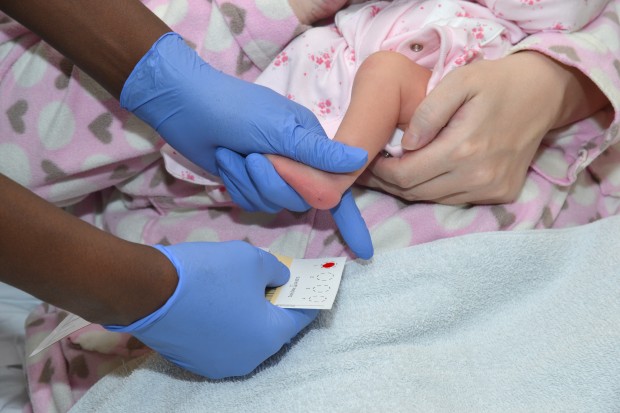
We’re pleased to say we have now published the revised newborn blood spot (NBS) screening standards, for implementation from 1 April 2020.
In July last year we asked for your views on proposed changes to the standards.
More than 100 people responded to the survey, and we’ve reviewed the comments and made some final changes using the PHE Screening standards framework.
Changes to the standards
You can find a summary of the changes in the supporting information and below. If you have any questions, please get in touch with us at the screening helpdesk.
Coverage (NBS-S01a and b)
The definitions of the coverage standards are now fully aligned with the coverage key performance indicators (KPI NB1 and NB4). They measure coverage of phenylketonuria (PKU) only.
Coverage data is collected through the KPI template only (quarterly data is combined to give the annual data for each provider).
Decline data will be collected in the KPI template to help interpret the coverage data.
The denominator for NBS-S01b (movers in) no longer includes the requirement for babies to have a blood spot sample taken before their first birthday, but the offer must still be made before their first birthday.
A new caveat reflects the revised policy on movers in with no available records. Screening should be offered to all babies under a year of age (up to but not including their first birthday) without documented results (or declines) for all 9 conditions. If screening is accepted, the sample must be taken no later than 14 calendar days after the baby’s first birthday. If your process is to offer and take the sample on the same day, this can only be done before the baby’s first birthday.
Checks for untested babies (NBS-S02)
There is no change to this standard for 2020. However, we’re planning to withdraw it when the revised child health information service specification is published. This is because we now consider this standard to be a structural standard.
Last year, all services that reported data met the acceptable threshold (by 17 days of age), and nearly 90% met the achievable threshold (by 14 days of age).
Barcoded NHS number labels (NBS-S03)
The numerator for this standard now only includes blood spot cards with a barcoded label that scans successfully in the laboratory.
Laboratories should feed back to maternity units when labels do not scan and give reasons (where it’s obvious) to help drive improvements.
There was mixed feedback on this in the consultation. After looking at it further, most laboratories reported that it was only practical to report the data in this way.
Timely sample collection and receipt in the newborn screening laboratory (NBS-S04 and S05)
We’ve updated the caveats – please see the supporting information.
Timely taking of a second blood spot sample for cystic fibrosis or congenital hypothyroidism screening (NBS-S07a, b, c)
We’ve paused these standards to review them further. A working group will look at the definitions, thresholds and benefits and burden of collecting the data in more detail.
The 2017 definitions will still be available, but will not be quality assured against or reviewed by screening and immunisation teams.
Timely processing of screen positive samples (NBS-S09)
We’ve updated the definition due to the different pattern of working days for some of the conditions.
Timely entry into clinical care (NBS-S11)
We’ve replaced the sickle cell disease thresholds with a link to the sickle cell and thalassemia standards.
Results to parents (NBS-S12a, b)
There’s no longer an exclusion for babies who have repeat samples. The thresholds have been lowered to ≥ 99.0% (acceptable) and ≥ 99.5% (achievable).
Laboratory accreditation (previous standards NBS-S08 and S10)
Laboratory accreditation will not be monitored through the programme screening standards. The programme is working with the screening quality assurance service (SQAS) to establish an appropriate reporting mechanism.
Proposed standard on sweat testing
We also asked for your views on introducing a standard on sweat testing (the gold standard diagnostic test for cystic fibrosis). We are not adding this to the standards at this time, but will ask our cystic fibrosis screening advisory board to review the comments.
Consultation report
Many thanks again to everyone who completed the consultation survey. You can access a copy of the consultation report by emailing the screening helpdesk.
PHE Screening blog
The PHE Screening blog provides up to date news from all NHS screening programmes. You can register to receive updates direct to your inbox, so there’s no need to keep checking for new blogs. If you have any questions about this blog article, or about population screening in England, please contact the PHE screening helpdesk.
Recent Comments