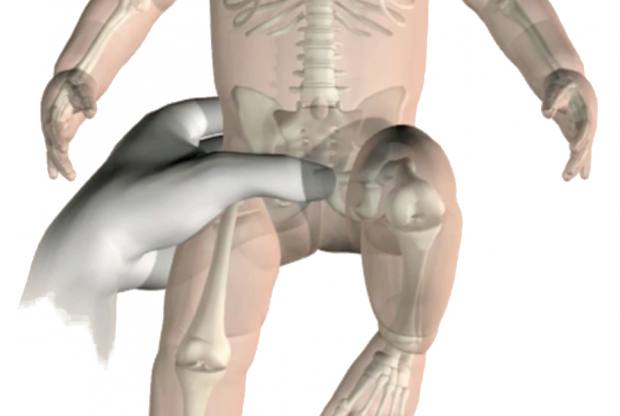
Developmental dysplasia of the hip (DDH) is a condition in which one or both hip joints fails to develop correctly.
About 1 to 2 in every 1,000 babies has DDH that requires treatment. Undetected DDH or delayed treatment can result in the need for complex surgery or long-term disability, pain and reduced quality of life.
Most babies who receive an early diagnosis and treatment develop normally, which is why screening is so important.
DDH is one of the conditions screened for by the NHS Newborn and Infant Physical Examination (NIPE) Programme. The NIPE screen at 72 hours checks for hip instability (see image above).
Babies who screen positive should be referred for an ultrasound scan by 2 weeks of age. Babies who have a normal clinical examination but also have risk factors for DDH need an additional ultrasound scan by 6 weeks of age.
Strengthening local screening pathways
A serious incident in one service in North Cumbria and the North East indicated there may be weaknesses in the NIPE pathway that might also be found in other trusts and could lead to babies with hip risk factors not receiving an ultrasound scan.
As a result, local antenatal and newborn screening coordinators agreed to take part in work to review and strengthen the pathway. The North Cumbria and North East Screening and Immunisation Team coordinated this work, supported by the national programme team and regional Screening Quality Assurance Service.
The screening coordinators completed an audit of all babies born within a one-year period who had a screen positive NIPE examination or presence of NIPE hip risk factors. This involved checking data from different local IT and manual clinical systems – and against the SMaRT4NIPE national IT system – to check babies had been managed correctly.
Sharing best practice
The work identified the following shared learning for local screening providers to note:
1. Review and standardise local training and ongoing competency assessment for NIPE practitioners, particularly across different professional groups.
2. Maternal obstetric history should be accessible and reviewed at the time of the examination, possibly using laptops that can be accessed at the bedside.
3. Make sure there is a clear understanding of who is responsible for completing and documenting NIPE pathways for babies who move between trusts in line with national guidance.
4. Make sure there is a clear trust policy for babies who are not brought to their appointments and clear documentation to prove the trust followed the local policy.
5. Have clear local processes for who inputs outcome data into SMaRT4NIPE, so that it serves as a failsafe against babies being missed. These processes should include contingency arrangements for when the failsafe officer, or other staff responsible for inputting outcomes into the system, are away.
The audit was a challenging but rewarding piece of work that has helped improve the NIPE pathways for babies born in North Cumbria and the North East. To find out more, please email england.cane.screeningimms@nhs.net.
PHE Screening blog
The PHE Screening blog provides up to date news from all NHS screening programmes. You can register to receive updates direct to your inbox, so there’s no need to keep checking for new blogs. If you have any questions about this blog article, or about population screening in England, please contact the PHE screening helpdesk.
Recent Comments