We get lots of questions about how to apply duty of candour regulations in screening programmes.
Duty of candour regulations require everyone to be open and honest with people who use our services and to say sorry when things go wrong.
I think we sometimes get into difficulties because it is the nature of all screening programmes that we can’t always detect all conditions all of the time. However, this doesn’t mean that screening programmes have done something wrong.
A false negative screening result is when a test indicates that an individual does not have the condition being screened for when, in reality, they do.
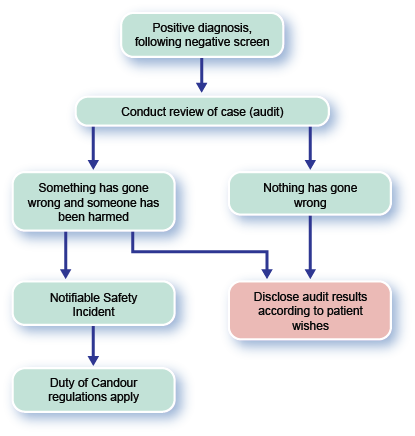
The 2 possible causes of a false negative result are:
- something has gone wrong
- everything was done correctly but our test wasn’t able to detect the condition this time (this happens in all screening programmes)
Determining which of the above situations applies is at the heart of deciding when to apply duty of candour regulations.
PHE Screening has worked with the Care Quality Commission (CQC), clinicians and patient representatives to put together new guidance to help organisations and clinicians decide how to interpret duty of candour in the context of a screening programme.
This guidance has built on a previous ‘Disclosure of Audit Guidance' best practice document produced by the cancer screening programmes.
Most of the questions we've received have come from radiologists and surgeons working in the NHS Breast Screening Programme who have asked for guidance about how to apply duty of candour to interval cancers. These are cancers that are diagnosed within the 3-year period after a normal (negative) screening result.
We've produced a number of resources for breast screening radiologists and surgeons explaining which types of interval cancer would be the subject of duty of candour and require the organisation to apologise to the patient for something having gone wrong.
Although many of the examples in the guidance are about breast screening we hope all clinicians working in screening will find the approach helpful in disclosing audit results and dealing with false negative screens.
We aim to publish more blogs and resources in future relating to duty of candour regulations in other screening programmes. If you have some suggestions relating to the programme you work in, or have examples you'd like us to work through, please contact the PHE Screening helpdesk.
PHE Screening blogs
PHE Screening BLOGs provide up to date news from all NHS screening programmes – replacing our previously published newsletters.
You can register to receive updates direct to your inbox, so there’s no need to keep checking for new blogs.